Varicose veins of the lower extremities are a problem that affects more than 60% of the world's population. The term "varicose veins" from the Latin "varix" is interpreted as "expansion". Hence the definition of the pathological condition - the expansion of the lumen of the veins of the lower extremities and pelvic organs, which significantly affects the flow of blood in the vessels and, accordingly, the general condition of theThe following material will consider the causes of varicose veins, possible complications of the disease, and the main ways of dealing with the pathology.
Causes and Risk Factors: Everyone is susceptible to this
Important:if varicose veins attack young people under the age of 25, then the gender distribution is 50: 50. That means boys and girls are equally ill. At a more mature age, women are more likely to have varicose veins due to pregnancy and age-related significant changes in hormone levels.
If you look at varicose veins from the inside, anatomically speaking, the venous lumen becomes enlarged due to a malfunction of the venous valves that regulate blood flow. Defective valves do not close completely with every heartbeat. As a result, blood coming out of the heart jerks to the lower extremities due to gravity.
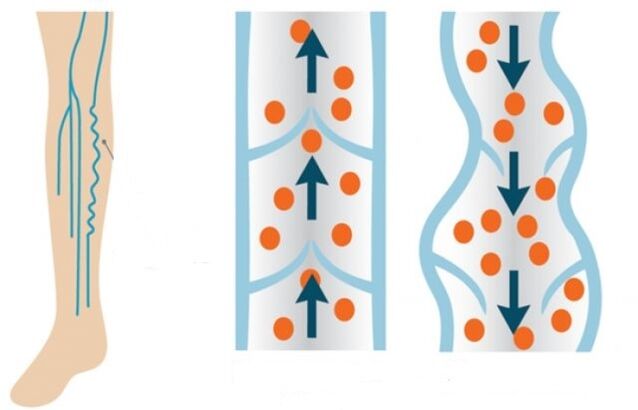
Normally, the valves should close and allow the blood to flow to the legs in portions. But unfortunately, the blood flow penetrates the legs more intensely, and in the opposite direction it moves less intensely due to the same poor functioning of the valve system. Leg veins that overflow with blood lose their elasticity and stretch.
The main predisposing factors for the development of a pathological condition of blood vessels are:
- genetic component (the disease can be transmitted within the family through the female or male line);
- Obesity;
- postponed pregnancies;
- passive lifestyle;
- excessive physical activity;
- Smoking and drinking alcohol;
- hormonal disorders.
Men problems
If you consider the causes of varicose veins depending on the gender of the patient, then they are slightly different in men and women. More precisely, each representative of different sexes is prone to certain habits that, sooner or later, can provoke the pathology of the vessels of the lower extremities. So risk factors for men are:
- Strength training with squat lifting;
- Overweight and obesity;
- unbalanced diet, which provokes frequent constipation;
- pathological processes of the kidneys (tumors of various etiologies);
- Inguinal hernia;
- sedentary work;
- Smoking and drinking alcohol.
Important:Men are characterized not only by the development of varicose veins of the lower extremities, but also by varicose veins of the spermatic cord. This pathology is called a varicocele. Such a condition is inherited, that is, it is exclusively genetic in nature and is not prevented even by increased preventive measures. Only 2-4% of men suffer from varicocele. The cause of the pathology is the asymmetrical anatomical location and structure of the male genital organs.
Due to the fact that men suffer from false shyness or do not have time to see a specialist at the onset of the disease, varicose veins are more difficult for them than for women.
Varicose veins in women have their own laws
Varicose veins are "better known" in women than in men. More than 80% of women suffer from vascular pathology of the legs. In addition, the risk group includes the fairer sex, who prefer this lifestyle or who suffer from the following conditions:
- wear tight high-heeled shoes;
- sitting or standing work;
- hereditary predisposition;
- Changes in hormone levels during pregnancy or with autoimmune diseases;
- wearing too tight underwear, jeans;
- Smoke;
- low proportion of fruits and vegetables in the diet (constant diets and hunger);
- Love of tanning (frequent visits to the solarium or staying in direct sunlight);
- severe weight gain;
- low mobility.
Pregnancy is where the "dog is buried"
Even if the manifestations of varicose veins, the causes and treatment of which should be established and prescribed only by a phlebologist, are initially not observed in a woman, then in 30% of cases it becomes apparent during pregnancy. Here the main trap lies in the growing fetus and with it in the uterus, which intensely compresses the pelvic organs. This significantly affects the blood circulation in the lower body. It is difficult for the blood to flow back up from the legs. This effect on the deep leg veins leads to the vessels being actively stretched in both width and length.
In addition to the growth of the uterine organ and pressure on the vessels of the pelvic organs, varicose veins in pregnant women also develop under the influence of such factors:
- Increased blood clotting. This is how nature insures a woman against major blood loss during childbirth. Thicker blood makes it harder to flow through the veins.
- An increase in progesterone hormone levels, which relaxes the muscles and blood vessels of the uterus so that it can rise freely and without tone as the fetus grows. At the same time, however, the walls of the other vessels also relax. The veins become less elastic and thick blood expands their walls, already weakened by progesterone, even more.
- Increase in blood pressure for better oxygen supply to the fetus. As a result, the body tries to quickly force thick blood through the relaxed vessels. This increases its volume in the legs.
- Low mobility of a pregnant woman with the growth of the abdomen. This leads to blood congestion in the legs and pelvic organs.
Complications from varicose veins
If varicose veins are not treated and observed, over time the patient can develop very serious complications, even requiring full-fledged surgical intervention. In the worst case, the patient can undergo an amputation of the affected limb. Below we consider the most common and dangerous complications of varicose veins.
Chronic venous insufficiency
With the development of such a complication, there is active failure of the venous valves. In addition, the pathological process is divided into four stages:
- Zero. The patient experiences slight swelling and rare pain in the legs after a hard day.
- First. The vein network of the enlarged vessels is visualized on the surface of the skin.
- Second. Swollen veins with blood clots and lumps are clearly visible. In places with inflamed veins, there is reddening, itching, wounds.
- Third. Trophic ulcers with inflamed veins form on the legs.
Important:Signs of chronic venous insufficiency are itching of the legs, pain, burning sensation when sitting for a long time, swelling, night cramps
Thrombophlebitis of the superficial veins
In this case, the patient develops a tendency to form blood clots. Clots actively block the lumen of the veins, making it difficult for blood to flow. In most cases, blood clots and clots are localized in the vessels of the lower third of the thigh or the upper third of the leg. The symptoms of venous thrombophlebitis are:
- Reddening of the skin of the legs in places of clot formation;
- Pain in the legs;
- on palpation - induration in the veins.
Important:with thrombophlebitis it is necessary to wear compression stockings. The compression formula should be selected by a specialist - angiosurgeon or phlebologist.
Trophic ulcer
This complication manifests itself in the later stages of venous insufficiency. Initially, the patient develops increased vascular permeability. A whitish seal with a varnish-like surface forms on the surface of the skin. An ulcer forms underneath. At the slightest injury to the inflamed area, the ulcer opens and exudate begins to discharge. The oozing wound can become infected secondarily, which leads to purulent inflammatory processes.
Important:In this condition, complete wound healing is required first and only then a full-fledged surgical procedure to remove the affected vessels.
Pulmonary embolism
An equally dangerous complication, in which a thrombus separates from the inflamed vein and migrates towards the pulmonary artery. This artery is directly involved in organizing blood flow in a small circle and affects the right ventricle of the heart. If the diameter of the detached thrombus is smaller than the lumen of the artery, the clot moves into the branches of the pulmonary artery and provokes pulmonary edema or infarction. In this case, the patient experiences significant chest pain. A wet cough mixed with blood, an increase in body temperature and weakness also occur. If the diameter of the clot is equal to the diameter of the lumen of the pulmonary artery, immediate blockage and death of the patient will result.
The detachment of a blood clot can be triggered by the following conditions:
- perform surgical interventions;
- Oncology;
- Heart failure;
- long bed rest.
Conservative and operative treatment
Varicose veins can be treated both conservatively and surgically, depending on the stage of the disease and the patient's condition. In the case of conservative treatment, the administration of phlebotonic drugs is indicated. Externally, gels and venotonic ointments based on horse chestnut are used. It should be understood that conservative treatment works only in the initial stages of varicose veins.
Physical activity (walking) and the wearing of compression stockings are shown as additional measures in the conservative treatment of varicose veins.
Minimally invasive and surgical treatment methods
When the process of varicose veins and venous insufficiency is far advanced, they resort to minimally invasive or full-fledged surgical interventions to improve the patient's condition. Minimally invasive intervention methods include:
- Sclerotherapy. A special sclerosing drug is injected into the lumen of the patient's varicose vein using a thin insulin needle. The injected substance causes inflammation and then sclerosis of the diseased vein. The lumen of the diseased vessel simply overgrows. The technique has more of a cosmetic effect, but does not solve the problem (the cause) of the pathology itself. Relapses are possible after sclerotherapy. Contraindications to such an intervention are pregnancy, lactation and intolerance to the components of the drug.
- Strip. With this method, the diseased vein is removed with the thinnest probe. The peculiarity of the surgical intervention is that only the diseased part of the vessel can be removed and the healthy parts are preserved. The operation is performed through two endoscopic punctures on either side of the site of the inflamed vessel. That is, scars and scars after such an operation are not visible.
- Microflebectomy. The diseased vein is also removed through several small incisions in the skin.
- Laser coagulation. Exposure of the lumen of a diseased vessel with a laser. This completely overgrows the lumen of the vein.
A full-fledged surgical procedure (abdominal surgery) is called a phlebectomy. In this method, the surgeon completely incises the skin of the leg to remove all of the superficial vein. The indications for such an operation are:
- a large volume of varicose veins;
- large cavity (lumen) of diseased vessels (more than 10 mm);
- Thrombophlebitis;
- the presence of large varicose veins;
- the formation of trophic ulcers in the patient;
- ineffectiveness of minimally invasive surgery.
Traditional methods of treatment
Also, at the initial stages of the pathology, you can resort to folk methods of treating varicose veins. In particular, when combined with drug treatment, you can use the following folk remedies:
- The tomato is green. Thin slices of vegetables are placed on the area of the inflamed veins and fixed with a bandage. You need to change such applications every 2-3 hours. The treatment is carried out until there is a clear improvement in the condition.
- Potatoes. A bandage soaked with freshly squeezed potato juice is applied to the legs. Cover the top with cling film. Such applications are best done at night until the patient's condition improves.
- Apple Cider Vinegar. Preferably homemade. Vinegar is diluted in water (1 glass of water and 2-3 tablespoons of vinegar). A bandage is moistened in a solution and applied to the area of the diseased veins. The bandage is fixed at night. You can easily lubricate your feet with this solution even at night. It is shown to take vinegar water and into it. Put 1 tablespoon of apple cider vinegar and a teaspoon of honey in a glass of water so as not to burn the esophagus with vinegar (the esophageal walls are very sensitive to acids). Drink the mixture in the morning on an empty stomach. Treatment with vinegar is 30 days.
- Buckeye. Flowers of the plant in the amount of 50 gr. Pour 0, 5 liters of alcohol and insist in a dark place for two weeks, periodically shaking the mixture. The finished product is filtered through a sieve and drunk three times a day, one tablespoon each time. The mixture is washed off with water. The duration of treatment is 7 days. Then a break of 14 days and again a seven-day course. Treatment according to this scheme is carried out until the end of the infusion. Then it can be prepared again and the therapy repeated.
- Burdock. In this case, fresh leaves of the plant are used to get rid of the disease. At night, sore feet are smeared with Vishnevsky's ointment and wrapped over it with a burdock leaf. All are fixed with a bandage and compression stockings are put on. The bandage is worn for three days, then it is removed and everything is washed off. It is possible to be treated this way all summer while fresh burdock is growing.
Important:such treatment is contraindicated in patients with high acidity of gastric juice.

Conclusions
It is worth noting that, in most cases, varicose veins are an irreversible pathology. That is why it is so important to take care of the health of your feet. Especially if there is a genetic predisposition to varicose veins. It is enough to give up bad habits, balance your daily diet, walk more, and drink enough clean water every day. At the manifestation of the slightest signs of varicose veins, it is advisable to immediately contact a competent phlebologist in order to avoid complications of the disease. Remember, your health and the internal health of your feet is entirely up to you. And modern medicine and the hands of a professional can work wonders.

























