Faced with a problem such as varicose veins of the lower extremities, the patient should not hesitate to see a doctor and begin treatment. An experienced specialist will conduct a thorough examination and draw conclusions as to which therapeutic tactic is best to choose: conservative or surgical treatment. If for some reason the medication is unable to have the desired effect on the patient's blood vessels, doctors will prescribe a surgical procedure that can already help unconditionally.
Indications and whether surgery is required at all
Surgery to remove varicose veins is a radical approach to the treatment of pathological vessels, so the indications for it are appropriate.

The operation is justified in the following cases:
- total varicose veins of the lower extremities that can be seen with the naked eye;
- constant severe swelling of the legs, discomfort, pain and heaviness in the legs or in other places depend on the localization of the pathological process;
- a direct danger that the existing varicose veins in a particular part of the body will be complicated by a more dangerous disease (e. g. thrombophlebitis, trophic ulcer, or pulmonary embolism).
In a direct conversation with the doctor, he can determine whether the operation is worthwhile and what types of surgical interventions are generally available.
Contraindications to the surgical treatment of varicose veins
Despite the strong indications, there are many cases when surgery to remove varicose veins on the legs can not be done. For example, if a patient has late stage varicose veins, surgical treatment is not always possible. In such cases, doctors rely on medication, but cannot provide sufficient help.
A number of other mandatory contraindications:
- the presence of skin diseases at the site of the affected vein, for example, eczema, pyoderma, dermatitis, etc.
- serious diseases of the cardiovascular system - hypertension, coronary artery disease, heart failure;
- acute inflammatory process in the vessel (phlebitis);
- previously transmitted thrombosis or pulmonary embolism;
- active process of eradicating atherosclerosis;
- older age;
- Period of pregnancy.
Patients should remember that if they are taking medication for other diseases, the attending physician must be notified.
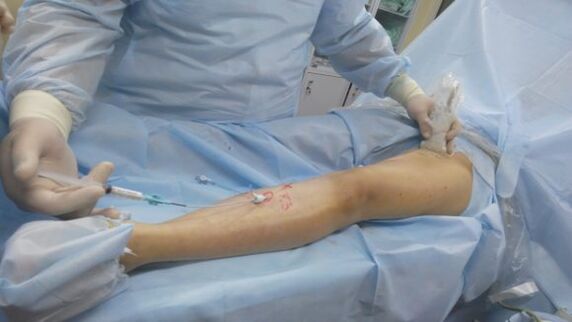
Sclerotherapy technique
Sclerotherapy is a procedure, the principle of which is to inject a special substance into the affected vessel, which causes further contraction and overgrowth of the vessel. The main advantage of this method is that the procedure does not require incisions or surgical access.
The gist of the procedure is as follows: the doctor, with the help of a syringe, injects a sclerosing substance into the pathological vessel. During one phase of sclerotherapy, a specialist will perform two to ten such injections. The effect does not appear at the same moment - it usually takes 2-8 weeks and several sessions of such a procedure. Under the action of sclerosant, the vein gradually narrows, then overgrows and disappears.
There are two types of manipulation:
- Microsclerosis. It is justified in the early stages of varicose veins, when small, superficial vessels are involved in the process. In such cases, the amount of sclerosant required is minimal.
- Echosclerosis. It is performed on deeper veins with duplex scanning in order to determine the location of deep varicose veins as precisely as possible.
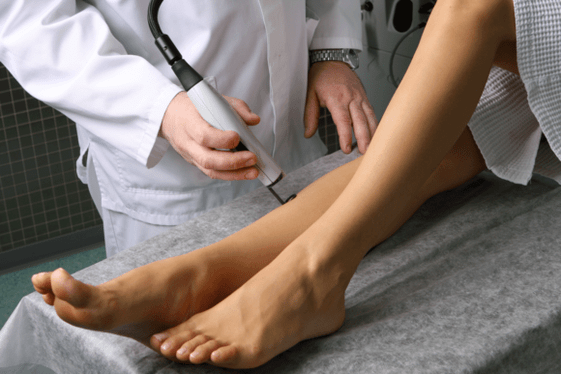
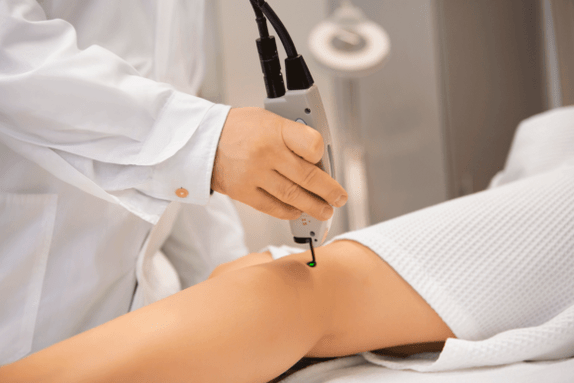
Laser coagulation
Laser surgery for varicose veins is by far the most popular. This is because the procedure itself is performed under local anesthesia, does not require large cuts and tissue trauma, and has an immediate effect.
The vascular surgeon should report in detail on how the operation was performed, but in general the essential thing is the introduction of a special laser light guide into the diseased vessel. A laser beam with its own wavelength penetrates this apparatus and acts on the walls of varicose veins. Under its action, the vessel coagulates and clogs.
This technique is justified if the patient has varicose veins in the leg or groin area. In addition, laser coagulation is more effective in large vessels, which is why the use of this technique is not justified in damage to small veins.
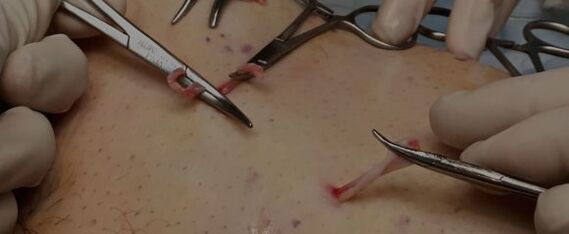
Ligation of veins
Vascular ligation is a more radical operation for varicose veins in the legs that requires a large incision and direct surgical access.
The operation is more often performed on the legs than on the vessels in the pelvic area. The technique of ligation of the saphenous vein will be effective. The vascular surgeon reaches into the indicated vessel at the point where the saphenous vein joins the femoral vein. Next, the surgeon bandages with special threads.
Pelvic vein surgery can be performed in women. In this case, the ovarian vein is made accessible and ligated.
Removal of dilated vessels
The most common and proven surgical method is phlebectomy. Doctors do it almost every day, and it's cheaper than laser coagulation or sclerotherapy. Such an operation for varicose veins is performed under general anesthesia or with epidural anesthesia.

To remove the dilated vessel, the surgeon needs an incision only 0. 5-1 cm long. After opening access to the area with varicose veins, the surgeon ligates, crosses, and removes the vessel.
Miniflebectomy is differentiated as a subtype of this procedure. It differs from conventional phlebectomy in that the surgeon requires punctures instead of incisions to gain access to the vessel. This surgery is effective for affecting small superficial vessels. Its main advantage is that it does not leave marks and cosmetic defects.
Stripping
Stripping is one of the subtypes of phlebectomy, which uses a special probe to remove a vein. As with the simple removal of varicose veins, the surgeon makes an incision in the trunk vein and accesses the vessel. Then the doctor makes another incision - in the middle or lower leg area.
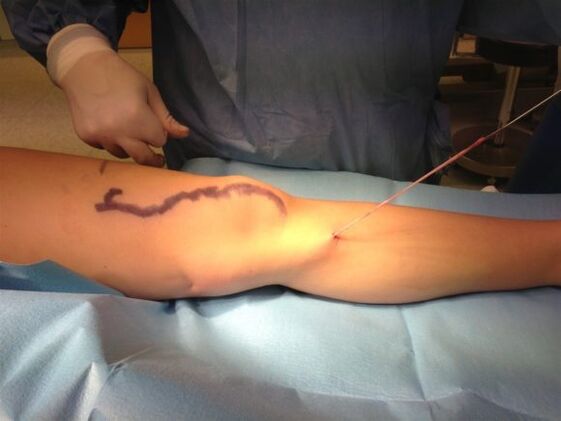
A special probe - an extractor probe - is inserted through the upper entrance into the great saphenous vein. The surgeon connects the mouth of the adjacent veins in front. The probe is passed the entire length of the vessel to the lower incision and then used to remove the vein.
A distinction is also made between several types of manipulation when stripping:
- Short stripping. Not the entire vessel is eliminated, but only a specific area that is subject to the varicose veins.
- Total. Such an operation on varicose veins of the lower extremities allows you to get rid of a large area of diseased vessels and avoid further relapses.
Consequences of surgery and rehabilitation
For varicose veins, surgery can have the opposite effect and cause various complications. They should be separated according to the type of procedure performed:

- After sclerotherapy, the patient may experience itching, burning, discoloration of the skin, and the appearance of edema at the injection site. An increase in body temperature and the appearance of general weakness are possible. Depending on the rules of the postoperative period, symptoms will go away in a couple of days.
- After laser coagulation, there may be a feeling of tension in the thigh area, slight bleeding and an increase in body temperature. With proper treatment, symptoms will go away within a week.
- Venous ligation can be complicated by trauma and bleeding during the surgery itself.
- Phlebectomy and stripping can damage the nerves in the skin. This can be accompanied by loss of sensitivity, numbness in the legs, and pain at the interfaces.
In all methods of surgical treatment, there is one common complication - thrombosis. This is a dangerous process, but the likelihood that it will occur as a result of surgery is very small.
In order to avoid the above complications and reduce your rehabilitation time as much as possible, it is necessary to adhere to the recommendations for taking care of your health and blood vessels in the postoperative period.
Depending on the rules of the postoperative period, symptoms will go away in a couple of days.
There are a number of pros and cons that are recommended by experts:
- Immediately after the end of the operation and for the first week after it, it is necessary to wear special compression underwear - this can be in the form of stockings, tights, socks, and for this purpose you can also use a normal elastic bandage.
- Eliminate bad habits - alcohol use, smoking, drug use.
- Avoid baths and saunas as well as baths that are too hot.
- In the place where the operation was performed, you can not perform cosmetic procedures and apply various cosmetics.
- Avoid strenuous physical activity. In the event that the patient did any kind of sport (especially hard) before the treatment, heavy loads should be forgotten for at least 5-8 weeks after the operation. In the future, you should consult with your doctor as to whether it is at all possible to continue vigorous exercise.
- Do prophylactic exercises every day that last no more than 15-30 minutes.
- To adhere to the phlebologist's prescriptions for taking medication - to take regular prophylactic anticoagulants, phlebotonics, non-steroidal anti-inflammatory drugs, thrombolytics and other drugs.
In general, all of these surgeries have good reviews from both doctors and patients. Which treatment approach is suitable for a particular patient only needs to be decided with the attending physician.

























