Varicose veins of the lower extremities are characterized by the expansion of the superficial leg veins, which is accompanied by the violation of blood flow in them and the failure of the valves. As a result, the veins increase in length and diameter, acquire a serpentine, cylindrical or sac-shaped appearance, although the listed deformities are also mixed.
Features of the venous system
The emergence and development of varicose veins is directly related to the venous system of the legs, which consists of:
- Saphenous veins: small and large;
- deep-set veins (in the lower leg and thigh);
- Perforating veins, which are the link between the two previous systems.
Normally 90% of the blood is transported to the lower extremities through deep veins and the remaining 10% through superficial ones. When it returns to the side of the heart, this mechanism is aided by valves in the vein walls. When the next serving of blood arrives, they strike to prevent their movement from top to bottom under the influence of gravity. Muscle contractions push the blood further towards the heart and allow normal blood flow.
With prolonged stay of a person in an upright position, blood stagnation may develop, which increases the pressure in the veins and increases their diameter. This process provokes an incomplete closure of the valve leaflets, as a result of which the flow of blood with its backflow from the heart - reflux - is disturbed.
The deep venous valves are most often affected, as they transport the largest amount of blood and thus experience the maximum stress. In order to reduce the high pressure in them, part of the blood is transported to the superficial ones via perforated veins, which were not originally intended for a large volume. Such a load on the vein walls leads to their expansion and the formation of varicose veins.
At the same time, blood penetrates the deep veins without interruption, but due to the violation of their functions and the normal activity of the valve cusps of the perforated veins, the blood is redistributed to the superficial vessels. As a result, chronic varicose veins develop, which over time are accompanied by painful sensations, edema and trophic ulcers.
Causes of the disease
One of the main causes of varicose veins used to be called hereditary factor, but today that theory has been refuted. Of course, it is possible to trace the common manifestations of the disease in some families, but this is more due to the peculiarities of life that are conveyed in the family: eating culture, passive rest, sedentary work and the like.
The formation of varicose veins is due to the presence of reflux in the venous system when the blood circulates through the veins in the opposite direction. Additional blood transport from deep veins to superficial veins is possible due to a congenital or acquired degenerative pathology of the valve apparatus. This leads to an overfilling of the superficial vessels with blood and their expansion when venous nodules form.
One of the main reasons for the development of varicose veins is considered to be an unhealthy diet, which in some cases leads to obesity. Such people exercise little, eat mostly highly processed foods, and minimize the amount of vegetable fiber in the diet. After all, it is they who are involved in strengthening the walls of veins and blood vessels and preventing persistent chronic constipation, which greatly increases intra-abdominal pressure, thereby provoking varicose veins. It should be noted that an increase in body weight of more than 20% increases the risk of disease five times.
The main provoking factor for women is carrying a child, while the risk of varicose veins increases with each subsequent pregnancy. Strong weight gain and an enlarged uterus put a lot of strain on the stagnant legs. This situation is aggravated by the ever-increasing intra-abdominal pressure and the action of the hormone progesterone, which affects the state of elastic fibers in the walls of blood vessels.
Other factors that provoke varicose veins of the lower extremities include:
- a sedentary lifestyle, standing upright during the day (e. g. hairdresser), long flights or long journeys. All this leads to stagnant processes in the lower extremities, when blood accumulates in the superficial veins and is poorly transported to the heart;
- sometimes increases the risk of developing varicose veins when women wear uncomfortable, tight shoes, especially models with high heels;
- Corsets and tight underwear compress the inguinal veins and increase intra-abdominal pressure, which is a direct prerequisite for varicose veins;
- high blood pressure;
- Smoking, which indirectly leads to a thinning of the walls of the blood vessels.
Classification of the disease
Varicose veins of the lower extremities are classified depending on the prevalence of venous lesions, their location, as well as the presence of pathological reflux, which is characterized by impaired blood flow. There are 4 types of varicose veins:
- intracutaneous and subcutaneous varicose veins (segmental), in which there is no pathological outflow of venous blood;
- segmental varicose veins, when reflux occurs through perforating or superficial veins;
- a common form of varicose veins in which reflux occurs simultaneously through the perforating and superficial veins;
- Varicose veins are characterized by reflux in deep veins.
After the varicose veins of the lower extremities become chronic, phlebology considers their three degrees:
- Transient edema, which regularly occurs against the background of the syndrome of "heavy legs".
- Persistent, persistent edema. Hyperpigmentation and eczema can occur.
- Venous ulcer of a trophic nature.
The latter degree is the most difficult to treat as it requires preliminary removal of the inflammation and healing of the skin tissue.
Stages and symptoms
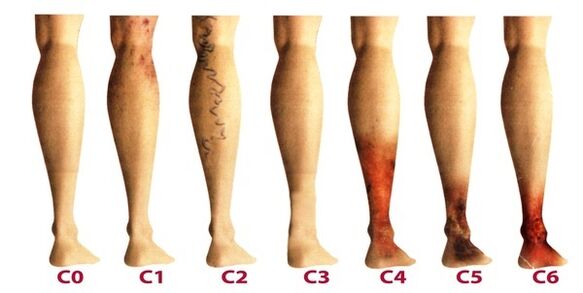
The disease develops very slowly, sometimes more than a dozen years pass before the symptoms that arise force the patient to seek advice from a phlebologist. In the early stages of varicose veins, their manifestations are often attributed to fatigue, age, or other reasons. In order to fully take into account the symptoms of the disease, its manifestations are classified according to the stages of the varicose veins:
- The first stage begins to manifest itself more often at a young age - after 20 years, when there is a feeling of heaviness in the legs, edema can appear, which completely disappears overnight. On the inside of the lower leg you can see an enlarged vein, which is expressed by a lumpy protrusion of skin. At this stage, many people notice small spider veins. In general, the symptomatology is subtle and rarely gets the attention it deserves.
- The second stage is characterized by an increase in the external manifestation of the dilated vein. The disease develops already against the background of the pathological work of the venous valves, therefore, the saphenous veins noticeably increase in size, and their elongation can also be noted. More often there is a feeling of heaviness and burning in the legs, they quickly get tired during long walks.
- The constant imbalance in the outflow of venous blood makes the disease already chronic. In the evening, patients suffer from edema near the ankle, which can be very intense. The legs are heavy and cramps can occur at night.
- Without treatment in the previous stages, chronic insufficiency of the functioning of the venous system negatively affects the metabolic processes in the skin, especially the areas in the lower part of the leg are affected. Near the ankle, darkening of the skin is visible - hyperpigmentation, it thickens and becomes inflamed over time. The condition described is called lipodermatosclerosis. If you do not start therapy related to the venous system at this time, trophic ulcers will soon form.
- The fifth stage is accompanied by numerous trophic ulcers, some of which regularly heal with scarring.
- In the zone of long-standing trophic disorders, extensive ulcers open. This condition requires urgent active therapy aimed at both the treatment of varicose veins and the healing of skin ulcers.
diagnosis
An external examination of the lower extremities in vertical and horizontal posture, palpation of the veins and a preliminary assessment of the disease stage are carried out. The patient is sent to a general blood test, which will allow you to more thoroughly examine the picture of the disease:
- a predisposition to thrombosis will be reflected at the platelet level;
- the hemoglobin level, as well as the number of red blood cells, indicate the degree of blood clotting;
- the increased white blood cell level can be used to assess inflammation, which helps diagnose thrombophlebitis more quickly.
Be sure to examine the venous system of the legs, for which there are many methods:
- Ultrasound Dopplerography - USDG;
- Venography;
- CT venography;
- Duplex angioscanning - USAS;
- Phleboscintiography;
- Photoplesmography;
- Phlebomanometry and the like.
In practice, USAS and USG are more often prescribed to patients because they help to fully examine the venous system of the legs and identify areas of degeneration. The remaining methods can also be prescribed if the ultrasound examination did not provide a complete view of the clinical picture. Some of these procedures can have complications such as venous thrombosis, perforation of the vessel wall with a catheter, and allergy to contrast media. Consider the most commonly practiced techniques in phlebology:
- USAS enables the assessment of the anatomical, hemodynamic and functional pathologies of the venous bed. The data obtained are subjected to computer processing, after which the model of the venous system can be viewed on video or printed out on paper.
- Doppler ultrasound with high accuracy determines the patency of superficial and deep-lying veins, the speed of blood flow. The Doppler ultrasound examination enables the function of the valve apparatus to be assessed.
After a detailed diagnosis, the doctor creates a phlebocard of the patient, which allows you to determine the damaged sections of the venous system, their degree and length. After that, a suitable treatment is selected.
treatment
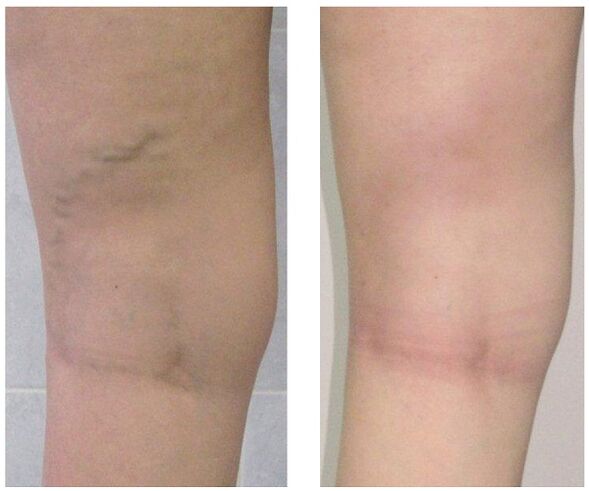
It is carried out extensively and depends on the symptoms, the degree of disease development and the results of the study. In the initial stages, conservative therapy is prescribed, which consists of:
- Drug treatment when prescribing a group of drugs:
- Antioprotectors and phlebotonics;
- Anticoagulants;
- Disaggregants
- topical preparations (ointments, gels);
- anti-inflammatory drugs.
- Elastic compression, for which compression stockings or bandages are (rarely) used. It allows you to dose the compression of the muscles, prevent stagnant processes and improve blood circulation in the vessels. When wearing such underwear, the vascular tone is artificially maintained.
- Physiotherapeutic methods, among which the best treatment results were shown by electrophoresis, diadynamic currents, laser radiation and magnetic field.
- Feasible physical activity that should only be done in compression garments (other than swimming). Cycling, swimming and jogging are recommended. The phlebologist selects an individual exercise set for the lower extremities that trains the vessels of the legs on a daily basis.
In addition, patients are recommended to perform contrasting five-minute procedures in the shower every evening, alternating between warm and cold water. Such manipulations improve blood flow and tone the blood vessels.
At the beginning of treatment, it is important to identify the disease-causing factor in order to be able to influence it effectively. And high-risk patients should visit a phlebologist every 2 years for a preventive examination and perform an ultrasound examination of the leg veins.
If conservative treatment does not bring results, or varicose veins are observed at an advanced stage, surgical intervention is performed. Today, varicose veins can be completely cured thanks to the following methods:
- Phlebectomy. The essence of the operation is to remove the main trunks of the superficial vein in order to eliminate the pathological outflow of blood. Perforating veins are often ligated for the same purpose.
- Sclerotherapy. It consists in the introduction of a sclerosant into the affected area of the vein, which leads to the connection of the walls. Recently, they began to actively use foamed sclerosant for the same purposes according to technology. The blood flow through the defective area stops and the cosmetic defect in the form of protruding nodules is eliminated. After such an operation, no scars remain, all manipulations are carried out on an outpatient basis without a subsequent inpatient stay. However, sclerotherapy is used only to fuse small branches of the venous trunks.
- Laser coagulation. With the help of a laser beam, the marked section of the vein is heated, the walls of which stick together and the blood flow stops. However, this technique is only indicated for veins with an expansion diameter of less than one centimeter.
prevention
Preventive measures can be both primary, to prevent the development of varicose veins, and secondary, when it is necessary to reduce the risk of relapse after surgery or to prevent the disease from worsening. Useful hints:
- lead an active lifestyle without putting too much strain on the legs: swimming, hiking, cycling;
- watch your weight;
- keep both legs raised more often;
- do not wear tight underwear and heels over 4 centimeters;
- use orthopedic insoles;
- take a contrast shower;
- do five-minute preventive leg exercises daily;
- Wear compression stockings for long walks.
If you notice the slightest suspicion of varicose veins - prominent nodules on the legs, swelling, heaviness, do not postpone the visit to the phlebologist. In fact, this insidious disease can provoke many complications over time, including thrombophlebitis and thrombosis.

























